Celiac Disease Presenting as Recurrent Pancreatitis and Pseudocyst
Abstract
Context The association between celiac disease and pancreatitis is sparsely reported. Celiac disease may remain asymptomatic or may have atypical features, and its diagnosis in pancreatitis may not be obvious. It is more than mere chance association that explains the occurrence of pancreatitis in celiac disease. Malnutrition, papillary stenosis and immunopathogenetic mechanisms contribute to the development of pancreatitis in a patient of celiac disease. Case report We here report one such case that had recurrent acute pancreatitis with pseudocyst formation and negative routine etiological work up. It was on noticing abnormal duodenal mucosa at the time of doing endoscopic cystogastrostomy that the diagnosis of celiac disease was suspected and later proved. Conclusion This report highlights that celiac disease should be considered in the etiological work up of patients with unexplained pancreatitis.
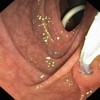
Image: Endoscopic image from second part of the duodenum showing grooving and nodularity in the duodenum.
Downloads
References
Lo W, Sano K, Lebwohl B, Diamond B, Green PH. Changing presentation of adult celiac disease. Dig Dis Sci. 2003 Feb;48(2):395-8.
Ludvigssons JF, Montgomery SM, Ekbom A et al. Risk of pancreatitis in 14,000 individuals with celiac disease. Clin Gastroenterol Hepatol 2007; 5:47-1353.
Ansaldi N, Oderda G. Exocrine pancreatic insufficiency in celiacsprue. Gastroenterology 1981; 80: 883.
Patel R, Johlin F, Murray J. Celiac disease and recurrent pancreatitis. Gastrointest Endosc 1999; 50: 823-827.
Sood A, Midha V, Sood N, et al. Coexistence of chronic calcific pancreatitis and celiac disease. Ind J Gastroenterol 2007; 26:41-2.
McManus R,Wilson AG, Mansfield J, et al. TNF2, a polymorphism of the tumour necrosis-alpha gene promoter, is a component of the celiac disease major histocompatibility complex haplotype. Eur J Immunol 1996; 26:2113-8.
Balog A, Gyulai Z, Boros LG, et al. Polymorphism of the TNFalpha, HSP70-2, and CD14 genes increases susceptibility to severe acute pancreatitis. Pancreas 2005; 30:e46-50.
Masoodi I, Wani H, Alsayari K, Sulaiman T, et al. Celiac disease and autoimmune pancreatitis: an uncommon association. A case report. Eur J GastroenterolHepatol. 2011;23:1270-2.
Carroccio A, Di Prima L, Scalici C, Soresi M et al. Unexplained elevated serum pancreatic enzymes: a reason to suspect celiac disease. Clin Gastroenterol Hepatol. 2006 Apr;4(4):455-9.
Kochhar R, Dutta U, Miglani A, Bhagat S, Poornachandra KS, Vaiphei K, et al. Celiac disease suspected at endoscopy in patients with chronic liver disease. Indian J Gastroenterol. 2011 Jul;30(4):166-9.
Dickey W. Diagnosis of coeliac disease at open-access endoscopy .Scand J Gastroenterol. 1998 Jun;33(6):612-5.
Bardella MT, Minoli G, Radaelli F, Quatrini M, et al. Reevaluation of duodenal endoscopic markers in the diagnosis of celiac disease. Gastrointest Endosc 2000 Jun;51(6):714-6.
Copyright (c) 2014 Jahangeer Basha, Sreekanth Appasani, Kim Vaiphei, Kartar Singh, Rakesh Kochhar

This work is licensed under a Creative Commons Attribution 4.0 International License.
As a member of Publisher International Linking Association, PILA, iMedPub Group’s JOP follows the Creative Commons Attribution License and Scholars Open Access publishing policies. Journal of the Pancreas is the Council Contributor Member of Council of Science Editors (CSE) and following the CSE slogan Education, Ethics, and Evidence for Editors.