A Pilot Retrospective Study of the Relationship Between Estrogen Use and Pancreatitis/Pancreatic Function in Women with Chronic Abdominal Pain
Abstract
Context Estrogens are thought to cause pancreatitis by raising triglyceride levels but whether there are other effects on the pancreas is debatable. Objective To better elucidate the relationship between estrogens and pancreatitis and pancreatic function in a pilot study. Design/setting/patients Our retrospectively collected database of 224 patients who had undergone secretin stimulation testing was queried for females with available medication histories, who were then divided into two groups: those taking estrogens (E) and those not on estrogens (N). Mann Whitney U and Fisher’s exact tests were used. Results Seventy of the patients in the database were females with available medication histories. Thirty-five (50.0%) were taking estrogens. Twenty-nine (82.9%) of the E patients experienced any type of pancreatitis (i.e., acute pancreatitis, acute relapsing pancreatitis, chronic pancreatitis) while only 19 (54.3%) of the N patients did (P=0.019). During secretin stimulation testing, the peak bicarbonate levels for E and N patients were 80±18 and 90±23 mEq/L, respectively (P=0.058). When patients with any type of pancreatitis were excluded, E patients still displayed decreased peak bicarbonate levels in response to secretin (90±18 vs. 104±19 mEq/L; P=0.021). Weight, age, triglyceride levels, frequency of patients with cholecystectomy and biliary stones did not significantly differ between the two groups (E and N respectively). Conclusions These pilot data suggest exogenous estrogens may be related to the development of acute pancreatitis and acute relapsing pancreatitis, and probably to a lesser degree chronic pancreatitis, perhaps through a triglyceride independent mechanism. During secretin stimulation testing, peak bicarbonate production may be diminished in women on estrogens (even in those who have never had pancreatitis). Further study is necessary to better define the relationship between estrogen use, pancreatitis, and pancreatic function.
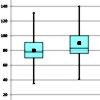
Image: Pancreatic function by peak bicarbonate.
Downloads
References
Tenner S. Drug-induced acute pancreatitis: underdiagnosis and overdiagnosis. Dig Dis Sci. 2010; 10:2706-8. PMID: 20686844
Nitsche CJ, Jamieson N, Lerch MM, Mayerle JV. Drug induced pancreatitis. Best Pract Res Clin Gastroenterol. 2010 ;24 :143-55. PMID: 22314811
Balani AR, Grendell JH. Drug-induced pancreatitis : incidence, management and prevention. Drug Saf. 2008; 31: 823-37. PMID: 18759507
Badalov N, Baradarian R, Iswara K, Li J, Steinberg W, Tenner S.Drug-induced acute pancreatitis: an evidence-based review. Clin Gastroenterol Hepatol. 2007; 5 :648-61; quiz 644. Review.PMID: 17395548
Lesser D, Hillesheim P. Pancreatitis in a woman taking an herbal supplement. South Med J. 2007; 100: 59-60. PMID: 17269527
Blake ED, Pitcher ME. Estrogen-related pancreatitis in the setting of normal plasma lipids: case report. Menopause 2003;10: 99–101. PMID: 12544683
Isley W, Oki J. Estrogen-induced pancreatitis after discontinuation of concurrent medroxyprogesterone therapy. Am J Med 1997; 102:416–417 PMID: 9217626
Tetsche MS, Jacobsen J, Nørgaard M, Baron JA, Sørensen HT. Postmenopausal hormone replacement therapy and risk of acute pancreatitis: a population-based case-control study. Am J Gastroenterol. 2007; 102: 275-8. PMID: 17311649
Lieb JG 2nd, Brensinger C, and Toskes PP. The Significance of the Volume of Pancreatic Juice Measured at Secretin Stimulation Testing: A Single Center Evaluation of 224 Classical Secretin Stimulation Tests. Pancreas. 2012 Apr 4. [Epub ahead of print] PMID: 22481285
Steer ML, Waxman I, Freedman S. Chronic pancreatitis. N Engl J Med. 1995; 332: 1482-90.
Kitagawa M, Naruse S, Ishiguro H, Nakae Y, Kondo T, Hayakawa T.Evaluating exocrine function tests for diagnosing chronic pancreatitis .Pancreas. 1997;15: 402-8.PMID: 9361095
Tuo B, Wen G, Wei J, Liu X, Wang X, Zhang Y, et al. Estrogen Regulation of Duodenal Bicarbonate Secretion and Sex-Specific Protection of the Human Duodenum. Gastro 2011; 141: 854-63. PMID: 21699784
Jowell PS, Branch MS, Fein SH, Purich ED, Kilaru R, Robuck G, et al. .Intravenous synthetic secretin reduces the incidence of pancreatitis induced by endoscopic retrograde cholangiopancreatography. Pancreas. 2011; 40: 533-9.PMID: 21499206
Lieb JG 2nd, Forsmark CE. A 50-year-old woman with unexplained recurrent pancreatitis. Clin Gastroenterol Hepatol. 2009; 7: 141-4. Epub 2008 Sep 3. PMID: 19187899
Anderson GL, Limacher M, Assaf AR, Bassford T, Beresford SA, Black H,et al; Women's Health Initiative Steering Committee.Effects of conjugated equine estrogen in postmenopausal women with hysterectomy: the Women's Health Initiative randomized controlled trial. .JAMA. 2004; 291: 1701-12.PMID: 15082697
Strom JO, Theodorsson A, Theodorsson E. Mechanisms of estrogens' dose-dependent neuroprotective and neurodamaging effects in experimental models of cerebral ischemia. Int J Mol Sci. 2011; 12: 1533-62. PMID: 21673906
Liarte S, Cabas I, Chaves-Pozo E, Arizcun M, Meseguer J, Mulero V, García-Ayala A. Natural and synthetic estrogens modulate the inflammatory response in the gilthead seabream (Sparus aurata L.) through the activation of endothelial cells. Mol Immunol. 2011; 48: 1917-25. PMID: 21683448
Knowlton AA, Lee AR. Estrogen and the cardiovascular system. Pharmacol Ther. 2012 Jul;135(1):54-70. Epub 2012 Mar 28. PMID: 22484805
Papachristou GI, Papachristou DJ, Avula H, Slivka A, Whitcomb DC. Obesity increases the severity of acute pancreatitis: performance of APACHE-O score and correlation with the inflammatory response.Pancreatology. 2006; 6: 279-85.PMID: 16636600
Williams G. Aromatase up-regulation, insulin and raised intracellular oestrogens in men, induce adiposity, metabolic syndrome and prostate disease, via aberrant ER-α and GPER signalling.Mol Cell Endocrinol. 2012; 351: 269-78. PMID: 22233684
Davis SR, Castelo-Branco C, Chedraui P, Lumsden MA, Nappi RE, Shah D, Villaseca P; as the Writing Group of the International Menopause Society for World Menopause Day 2012. Understanding weight gain at menopause. Climacteric. 2012 Oct;15(5):419-29.PMID: 22978257
Forsmark CE, Baillie J, AGA Institute Clinical Practice and Economics Committee, AGA Institute Governing Board AGA Institute technical review on acute pancreatitis. Gastroenterology. 2007;132: 2022-44. PMID: 17484894
Copyright (c) 2014 John George Lieb II, Phillip P Toskes

This work is licensed under a Creative Commons Attribution 4.0 International License.
As a member of Publisher International Linking Association, PILA, iMedPub Group’s JOP follows the Creative Commons Attribution License and Scholars Open Access publishing policies. Journal of the Pancreas is the Council Contributor Member of Council of Science Editors (CSE) and following the CSE slogan Education, Ethics, and Evidence for Editors.