Autoimmune Pancreatitis Complicated by Spontaneous Subcapsular Splenic Haemorrhage
Abstract
Context Autoimmune pancreatitis is a rare but increasingly recognised condition with unique clinical, immunological and histological features. We report the first case of autoimmune pancreatitis associated with spontaneous splenic haemorrhage. Case report A 75-year-old man presented with severe epigastric pain radiating to the back associated with nausea and vomiting. A CT-scan of his abdomen showed a large pseudocyst within the pancreatic tail as well as a subcapsular splenic haemorrhage. His IgG4 levels were elevated and clinical history and investigations were consistent with severe acute pancreatitis, but were negative for other known causes of pancreatic disease. The patient was started on steroid therapy and improved dramatically clinically, immunologically and radiologically thus confirming the diagnosis of autoimmune pancreatitis. His splenic haemorrhage was managed conservatively in view of his haemodynamic stablity and eventually self-resolved. Conclusion Autoimmune pancreatitis should not be overlooked in cases of acute pancreatitis without other obvious etiology. Furthermore, superimposed splenic haemorrhage is a rare but important complication of autoimmune pancreatitis.
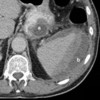
Image: CT scan showing a large pseudocyst and subcapsular splenic haemorrhage.
Downloads
References
Banks PA, Bollen TL, Dervenis C, Gooszen HG, Johnson CD, Sarr MG, et al. Classification of acute pancreatitis-2012: revision of the Atlanta classification and definitions by international consensus. Gut 2013; 62:102-11. [PMID: 23100216]
Chari ST. Diagnosis of autoimmune pancreatitis using its five cardinal features: introducing the Mayo Clinic's HISORt criteria. J Gastroenterol 2007; 42(Suppl 18):39-41. [PMID: 17520222]
Gardner TB, Levy MJ, Takahashi N, Smyrk TC, Chari ST. Misdiagnosis of autoimmune pancreatitis: a caution to clinicians. Am J Gastroenterol 2009; 104:1620-3. [PMID: 19574965]
Shimosegawa T, Chari ST, Frulloni L, Kamisawa T, Kawa S, Mino-Kenudson M, et al. International consensus diagnostic criteria for autoimmune pancreatitis: guidelines of the International Association of Pancreatology. Pancreas 2011; 40:352-8. [PMID: 21412117]
Sugumar A, Smyrk TC, Takahashi N, et al. Lymphoplasmacytic sclerosing pancreatitis (LPSP) and idiopathic duct centric pancreatis (IDCP) are distinct clinical forms of autoimmune pancreatitis (AIP). Pancreas 2008; 37:497.
Sah RP, Chari ST, Pannala R, Sugumar A, Clain JE, Levy MJ, et al. Differences in clinical profile and relapse rate of type 1 versus type 2 autoimmune pancreatitis. Gastroenterology 2010; 139:140-8. [PMID: 20353791]
Sugumar A, Kloppel G, Chari ST. Autoimmune pancreatitis: pathologic subtypes and their implications for its diagnosis. Am J Gastroenterol 2009; 104:2308-10. [PMID: 19727085]
Law R, Bronner M, Vogt D, Stevens T. Autoimmune pancreatitis: a mimic of pancreatic cancer. Cleve Clin J Med 2009; 76:607-15. [PMID: 19797461]
Pearson RK, Longnecker DS, Chari ST, Smyrk TC, Okazaki K, Frulloni L, Cavallini G. Controversies in clinical pancreatology: autoimmune pancreatitis: does it exist? Pancreas 2003; 27:1-13. [PMID: 12826899]
Pezzilli R. Acute recurrent pancreatitis: An autoimmune disease? World J Gastroenterol 2008; 14: 999-1006. [PMID: 18286678]
Muraki T, Hamano H, Ochi Y, et al. Corticosteroid-responsive pancreatic cyst found in autoimmune pancreatitis. J Gastroenterol 2005; 40:761-6. [PMID: 16082595]
Mortele KJ, Mergo PJ, Taylor HM, et al. Splenic and perisplenic involvement in acute pancreatitis: determination of prevalence and morphological helical CT features. J Comput Assist Tomogr 2001; 25:50-4. [PMID: 11176293]
Kurzbaum A, Lieberman L, Qarawany M, Nasrallah N, Safori G. Spontaneous splenic rupture: A rare complication of chronic pancreatitis. Israeli Journal of Emergency Medicine 2008; 8 :35-8.
Patil PV, Khalil A, Thaha MA. Splenic parenchymal complications in pancreatitis. JOP. J Pancreas (Online) 2011; 12:287-91. [PMID: 21546711]
Copyright (c) 2014 Mina S Hanna, Ana Terlevich, Robert Przemioslo, Peter Marden

This work is licensed under a Creative Commons Attribution 4.0 International License.
As a member of Publisher International Linking Association, PILA, iMedPub Group’s JOP follows the Creative Commons Attribution License and Scholars Open Access publishing policies. Journal of the Pancreas is the Council Contributor Member of Council of Science Editors (CSE) and following the CSE slogan Education, Ethics, and Evidence for Editors.