Pancreatic Metastasis from a Solitary Fibrous Tumor of the Central Nervous System
Abstract
Context Solitary fibrous tumor of the central nervous system is uncommon, with only around 200 reported cases. Further, extracranial metastasis is extremely rare, and only 5 cases of hematogenous metastases have been reported so far. To the best of our knowledge, there have been no reports of solitary fibrous tumor of the central nervous system metastasizing to the pancreas. Case report A 62-year-old woman was referred for evaluation of a pancreatic mass, which was strongly suspected to be a neuroendocrine tumor. However, the histological findings and immunohistochemical profile indicated the presence of a solitary fibrous tumor. Because the medical history revealed previous transcranial resection for intracranial meningioma 16 years ago, we conducted a pathological review of the brain specimen obtained by the first operation and found that it had the same histology and immunohistochemical profile as the current endoscopic ultrasound-guided fine-needle aspiration specimen. Consequently, the final diagnosis, on the basis of the brain specimen, was changed from meningioma to solitary fibrous tumor of the central nervous system, and the pancreatic mass was diagnosed as metastasis from solitary fibrous tumor of the central nervous system. The patient underwent middle pancreatectomy; the pancreatic specimen also had the same histology and immunohistochemical profile as the brain specimen. Conclusion Histological findings and immunohistochemical profile obtained by EUS-FNA are invaluable for the correct diagnosis to avoid excessive surgical procedures.
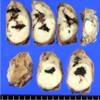
Image: Middle pancreatectomy specimen.
Downloads
References
Carneiro SS, Scheithauer BW, Nascimento AG, et al. Solitary fibrous tumor of the meninges: a lesion distinct from fibrous meningioma. A clinicopathologic and immunohistochemical study. Am J Clin Pathol.1996; 106: 217-224.
Bisceglia M, Galliani C, Giannatempo G et al. Solitary fibrous tumor of the central nervous system: a 15-year literature survey of 220 cases (August 1996-July 2011). Adv Anat Pathol. 2011; 18: 356-392.
Bisceglia M, Dimitri L, Giannatempo G et al. Solitary fibrous tumor of the central nervous system: report of an additional 5 cases with comprehensive literature review. Int J Surg Pathol. 2011; 19: 476-486.
Chen H, Zeng XW, Wu JS et al. Solitary fibrous tumor of the central nervous system: a clinicopathologic study of 24 cases. Acta Neurochir. 2012; 154: 237-248.
Ng HK, Choi PC, Wong CW, et al. Metastatic solitary fibrous tumor of the meninges. Case report. J Neurosurg. 2000; 93: 490-493.
Kim KA, Gonzalez I, McComb JG, et al. Unusual presentations of cerebral solitary fibrous tumors: report of four cases. Neurosurgery. 2004; 54: 1004-1009.
Ogawa K, Tada T, Takahashi S, et al. Malignant solitary fibrous tumor of the meninges. Virchows Arch. 2004; 444: 459-464.
Metellus P, Bouvier C, Guyotat J, et al. Solitary fibrous tumors of the central nervous system: clinicopathological and therapeutic consideration of 18 cases. Neurosurgery. 2007; 60: 715-722.
Muñoz E, Prat A, Adamo B, et al. A rare case of malignant solitary fibrous tumor of the spinal cord. Spine. 2008; 33: E397-399.
Klemperer P, Rabin CB. Primary neoplasms of the pleura; a report of five cases. Arch Pathol. 1931; 11: 385-412.
Rodriguez-Gil Y, ZGonzalez MA, Carcavilla CB et al. Lines of cell differentiation in solitary fibrous tumor: an ultrastructural and immunohistochemical study of 10 cases. Ultrastruct Pathol. 2009; 33:274-85.
Louis DN, Ohgaki H, Wiestler OD, Cavenee WK. WHO classification of tumours of the central nervous system. Lyon: IARC; 2007.
Ambrosini-Spaltro A, Eusebi V. Meningeal hemangio-pericytomas and hemangiopericytoma/solitary fibrous tumors of extracranial soft tissues: a comparison. Virchows Arch. 2010; 456: 343-354.
Cummings TJ, Burchette JL, McLendon RE. CD34 and dural fibroblasts: the relationship to solitary fibrous tumor and meningioma. Acta Neuropathol. 2001; 102: 349-354.
Sundin A, Vullierme MP, Kaltsas G, et al. ENETS Consensus Guidelines for the Standards of Care in Neuroendocrine Tumors: radiological examinations. Neuroendocrinology. 2009; 90: 167-183.
Crippa S, Angelini C, Mussi C, et al. Surgical treatment of metastatic tumors to the pancreas: a single center experience and review of the literature. World J Surg. 2006; 30: 1536–1542.
Srinivasan V, Wayne J, Rao M, et al. Solitary fibrous tumor of the pancreas: case report with cytologic and surgical pathology correlation and review of the literature. J Pancreas. 2008; 9: 526–530.
Ishiwatari H, Hayashi T, Yoshida M, et al. A case of solitary fibrous tumor of the pancreas. Nippon Shokakibyo Gakkai Zasshi. 2009; 106: 1078-1085.
Suzuki S, Kaji S, Koike N, et al. Pancreatic schwannoma: a case report and literature review with special reference to imaging features. JOP. 2010; 8: 31-35.
Somashekar GK, Muhannad MH, Shree GS, et al. Intrapancreatic Accessory Spleen: Investigative Dilemmas and Role of EUS-Guided FNA for Diagnostic Confirmation. JOP. 2011; 12: 603-606.
Gilbert CM, Monaco SE, Cooper ST, et al. Endoscopic ultrasound fine-needle aspiration of metastases to the pancreas: A study of 25 cases. Cytojournal. 2011; 8: 7.
Falconi M, Bartsch DK, Eriksson B, Klöppel G, et al. ENETS Consensus Guidelines for the management of patients with digestive neuroendocrine neoplasms of the digestive system: well-differentiated pancreatic non-functioning tumors. Neuroendocrinology. 2012; 95: 120-134.
Cauley CE, Pitt HA, Ziegler KM, et al. Pancreatic enucleation: improved outcomes compared to resection. J Gastrointest Surg. 2012; 16: 1347-53.
Hirono S, Yamaue H. Middle pancreatectomy for pancreatic neoplasms. J Hepatobiliary Pancreat Sci. 2010;17: 803-807.
Keck T, Adam U, Makowiec F, et al. Short- and long-term results of duodenum preservation versus resection for the management of chronic pancreatitis: a prospective, randomized study. Surgery. 2012; 152: S95-S102.
Copyright (c) 2014 Takahiro Osuga, Tsuyoshi Hayashi, Hirotoshi Ishiwatari, Michihiro Ono, Makoto Yoshida, Yasutoshi Kimura, Tadashi Hasegawa, Yasushi Sato, Tsutomu Sato, Koji Miyanishi, Rishu Takimoto, Masayoshi Kobune, Junji Kato

This work is licensed under a Creative Commons Attribution 4.0 International License.
As a member of Publisher International Linking Association, PILA, iMedPub Group’s JOP follows the Creative Commons Attribution License and Scholars Open Access publishing policies. Journal of the Pancreas is the Council Contributor Member of Council of Science Editors (CSE) and following the CSE slogan Education, Ethics, and Evidence for Editors.