Sporadic Insulinoma in a 10-Year-Old Boy: A Case Report and Literature Review
Abstract
Context Insulinoma is an exceedingly uncommon pancreatic islet cell neuroendocrine tumor. Its estimated incidence is approximately four cases per million individuals per year. Case report We report the case of sporadic insulinoma in an exceptionally very young 10-year-old boy who presented with a 1-month history of episodic tremulousness, diaphoresis, increased hunger, confusion and fainting. Initial laboratory investigations showed low blood glucose (64 mg/dL) and high blood insulin (6 μU/mL) levels. Patient was admitted in view of frequent hypoglycemic symptoms and possible pancreatic insulinoma. A 48-hour mentored fasting test was done and ceased within 3 hours due to occurrence of hypoglycemic symptoms. During the episode, blood was drawn and results showed low blood glucose level and high insulin, pro-insulin and C-peptide levels. The hypoglycemic symptoms were relieved greatly by glucose administration and Whipple’s triad for insulinoma was met. An abdominal contrast-enhanced computed tomography scan showed a 10x12x17 mm, small, well-demarcated, heterogeneously enhancing lesion within the body of pancreas without dilatation of pancreatic duct. No evidence of lymphadenopathy or distant metastasis was identified. Patient underwent enucleation of pancreatic tumor. Histopathological and immunohistochemical examination of the pancreatic mass confirmed neuroendocrine tumor (insulinoma). Patient had an uneventful recovery. A post-operative 6-month follow-up showed resolution of hypoglycemic symptoms, normalized blood glucose, insulin, pro-insulin and C-peptide levels, and no evidence of recurrence. Conclusion Although rare, sporadic insulinoma should be considered in the differential diagnosis of any young individual presenting with frequent hypoglycemic symptoms (neuroglycopenic and/or autonomic nervous system symptoms). Furthermore, a literature review on insulinoma is presented.
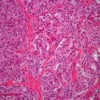
Image: Cells organized in solid trabeculae or nests separated by fibrovascular stroma.
Downloads
References
Service FJ, McMahon MM, O’Brien PC, Ballard DJ. Functioning insulinoma: incidence, recurrence and long-survival of patients: a 60-year study. Mayo Clin Proc. 1991;66(7):711-9.
Jani N, Moser AJ, Khalid A. Pancreatic endocrine tumors. Gastroenterol Clin North Am. 2007;36(2):431-9, x-xi.
Stephen AE, Hodin RA. Neuroendocrine tumors of the pancreas, excluding gastrinoma. Surg Oncol Clin N Am. 2006;15(3):497-510.
Grant CS. Insulinoma. Best Pract Res Clin Gastroenterol. 2005;19(5):783-98.
Oberg K, Eriksson B. Endocrine tumours of the pancreas. Best Pract Res Clin Gastroenterol. 2005;19(5):753-81.
Tucker ON, Crotty PL, Conlon KC. The management of insulinoma. Br J Surg. 2006; 93(3):264-75.
Abbasakoor NO, Healy ML, O'Shea D, et al. Metastatic insulinoma in a patient with type 2 diabetes mellitus: case report and review of the literature. Int J Endocrinol. 2011;2011:124078.
Yao JC, Rindi G, Evans DB. Pancreatic endocrine tumors. In: Devita VT Jr, Hellman S, Rosenberg SA, editors. Cancer principles and practice of oncology. 8th edition. Philadelphia, USA: Lippincott Williams & Wilkins; 2007: 1702-1716.
Hirshberg B, Livi A, Bartlett DL, et al. Forty-eight-hour fast: the diagnostic test for insulinoma. J Clin Endocrinol Metab. 2000;85(9):3222-6.
Whipple AO, Frantz VK. Adenoma of islet cells with hyperinsulinism: a review. Ann Surg. 1935; 101(6):1299–1335.
Boukhman MP, Karam JH, Shaver J, Siperstein AE, Duh QY, Clark OH. Insulinoma—experience from 1950 to 1995. West J Med. 1998;169(2):98-104.
Service FJ. Diagnostic approach to adults with hypoglycemic disorders. Endocrinol Metab Clin North Am. 1999;28(3):519-32, vi.
McLean A. Endoscopic ultrasound in the detection of pancreatic islet cell tumours. Cancer Imaging. 2004;4(2):84-91.
Vaidakis D, Karoubalis J, Pappa T, Piaditis G, Zografos GN. Pancreatic insulinoma: current issues and trends. Hepatobiliary Pancreat Dis Int. 2010;9(3):234-41.
Finlayson E, Clark OH. Surgical treatment of insulinomas. Surg Clin North Am. 2004;84(3):775-85.
Oberg K. Pancreatic endocrine tumors. Semin Oncol. 2010;37(6):594-618.
Lack EE. Pancreatic endocrine neoplasms. In: Lack EE, editor. Pathology of the pancreas, gallbladder, extrahepatic biliary tract and ampullary region. New York, USA: Oxford University Press; 2003: 323–373.
de Herder WW, Niederle B, Scoazec JY, et al. Well-differentiated pancreatic tumor/ carcinoma: insulinoma. Neuroendocrinology. 2006;84(3):183-8.
Cohen MS, Bower RH, Fidler SM, Johnsonbaugh RE, Sode J. Inhibition of insulin release by diphenylhydantoin and diazoxide in a patient with benign insulinoma. Lancet. 1973;1(7793):40-1.
Hirshberg B, Cochran C, Skarulis MC, et al. Malignant insulinoma: spectrum of unusual clinical features. Cancer. 2005;104(2):264-72.
Norton JA, Cromack DT, Shawker TH, et al. Intraoperative ultrasonographic localization of islet cell tumors. A prospective comparison to palpation. Ann Surg. 1988;207(2):160-8.
Copyright (c) 2014 Ahmed Abu-Zaid, Lama Abdulhamid Alghuneim, Mona Tarek Metawee, Ragaa Osama Elkabbani, Hadeel Almana, Tarek Amin, Ayman Azzam

This work is licensed under a Creative Commons Attribution 4.0 International License.
As a member of Publisher International Linking Association, PILA, iMedPub Group’s JOP follows the Creative Commons Attribution License and Scholars Open Access publishing policies. Journal of the Pancreas is the Council Contributor Member of Council of Science Editors (CSE) and following the CSE slogan Education, Ethics, and Evidence for Editors.