Synchronous Presentation of Ampullary Adenocarcinoma and Common Bile Duct Cancer: Report of a Case and Review of Literature
Abstract
Context Ampullary adenocarcinomas and bile duct cancers represent a very small minority of all gastrointestinal malignancies. Synchronous presentation of both malignancies is extremely rare. Case report We report a case of a 76-year-old male who presented with painless jaundice. His work-up showed an ampullary mass and a separate common bile duct stricture. Attempted endoscopic resection established the diagnosis of ampullary adenocarcinoma. Pathologic examination of the Whipple specimen identified a separate focus of bile duct cancer. Conclusion Synchronous presentation of an ampullary mass and separate distal bile duct stricture, especially in elderly patients, should raise concern for both lesions representing malignancies. In the absence of conclusive evidence for survival advantage in resected early stage ampullary and biliary cancers, close observation should be considered a valid alternative to adjuvant chemotherapy and radiation.
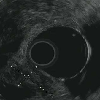
Image: EUS showing a hypoechoic oval mass in the ampulla.
Downloads
References
Kim RD, Kundhal PS, McGilvray ID, et al. Predictors of failure after pancreaticoduodenectomy for ampullary carcinoma. J Am Coll Surg 2006;202:112–119.
Howe JR, Klimstra DS, Moccia RD, Conlon KC, Brennan MF. Factors predictive of survival in ampullary carcinoma. Ann Surg. 1998;228:87-94.
Albores-Saavedra J, Schwartz AM, Batich K, Henson DE. Cancers of the ampulla of vater: demographics, morphology, and survival based on 5,625 cases from the SEER program. J Surg Oncol. 2009;100:598-605.
Yeo CJ, Sohn TA, Cameron JL, Hruban RH, Lillemoe KD, Pitt HA. Periampullary adenocarcinoma: analysis of 5-year survivors. Ann Surg. 1998;227:821-31.
Carter JT, Grenert JP, Rubenstein L, et al. Tumors of the ampulla of vater: histopathologic classification and predictors of survival. J Am Coll Surg. 2008;207:210-8.
Lack E. “Pathology of the Extrahepatic Biliary Tract and Ampullary Region” in Pathology of the Pancreas, Gallbladder, Extrahepatic Biliary Tract, and Ampullary Region, Oxford University Press, 2003
American Joint Committee on Cancer. “Tumors of the Ampulla of Vater” in AJCC Cancer Staging Manual, Seventh Edition, Springer 2010
Odze RD and Goldblum JR. “Epithelial Neoplasms of the Small Intestine” in Surgical Pathology of the GI Tract, Liver, Biliary Tract and Pancreas, Saunders 2009
Zhou H. Schaefer N, Wolff M, Fischer HP. Carcinoma of the ampulla of Vater: comparative histologic/immunohistochemical classification and followup. Am J Surg Pathol 2004; 28:875-882
Chu PG, Schwarz RE, Lau SK, Yen Y, Weiss LM. Immunohistochemical staining in the diagnosis of pancreaticobiliary and ampulla of Vater adenocarcinoma. Application of CDX2, CK17, MUC1 and MUC2. Am J Surg Pathol 2005; 29:359-367
Duffy JP, Hines OJ, Liu JH, et al. Improved survival for adenocarcinoma of the ampulla of Vater: fifty-five consecutive resections. Arch Surg. 2003;138:941-8; discussion 948-50.
Beger HG, Treitschke F, Gansauge F, Harada N, Hiki N, Mattfeldt T. Tumor of the ampulla of Vater: experience with local or radical resection in 171 consecutively treated patients. Arch Surg. 1999;134:526-32.
Winter JM, Cameron JL, Olino K, et al. Clinicopathologic analysis of ampullary neoplasms in 450 patients: implications for surgical strategy and long-term prognosis. J Gastrointest Surg. 2010;14:379-87.
Valle J, Wasan H, Palmer DH, et al. Cisplatin plus gemcitabine versus gemcitabine for biliary tract cancer. N Engl J Med. 2010;362:1273-81.
Klinkenbijl JH, Jeekel J, Sahmoud T, et al. Adjuvant radiotherapy and 5-fluorouracil after curative resection of cancer of the pancreas and periampullary region: phase III trial of the EORTC gastrointestinal tract cancer cooperative group. Ann Surg 1999;230:776-82, discussion 782-4.
Copyright (c) 2014 Max V Wohlauer, Martine C McManus, Brian Brauer, Jeremy Hedges, Csaba Gajdos

This work is licensed under a Creative Commons Attribution 4.0 International License.
As a member of Publisher International Linking Association, PILA, iMedPub Group’s JOP follows the Creative Commons Attribution License and Scholars Open Access publishing policies. Journal of the Pancreas is the Council Contributor Member of Council of Science Editors (CSE) and following the CSE slogan Education, Ethics, and Evidence for Editors.